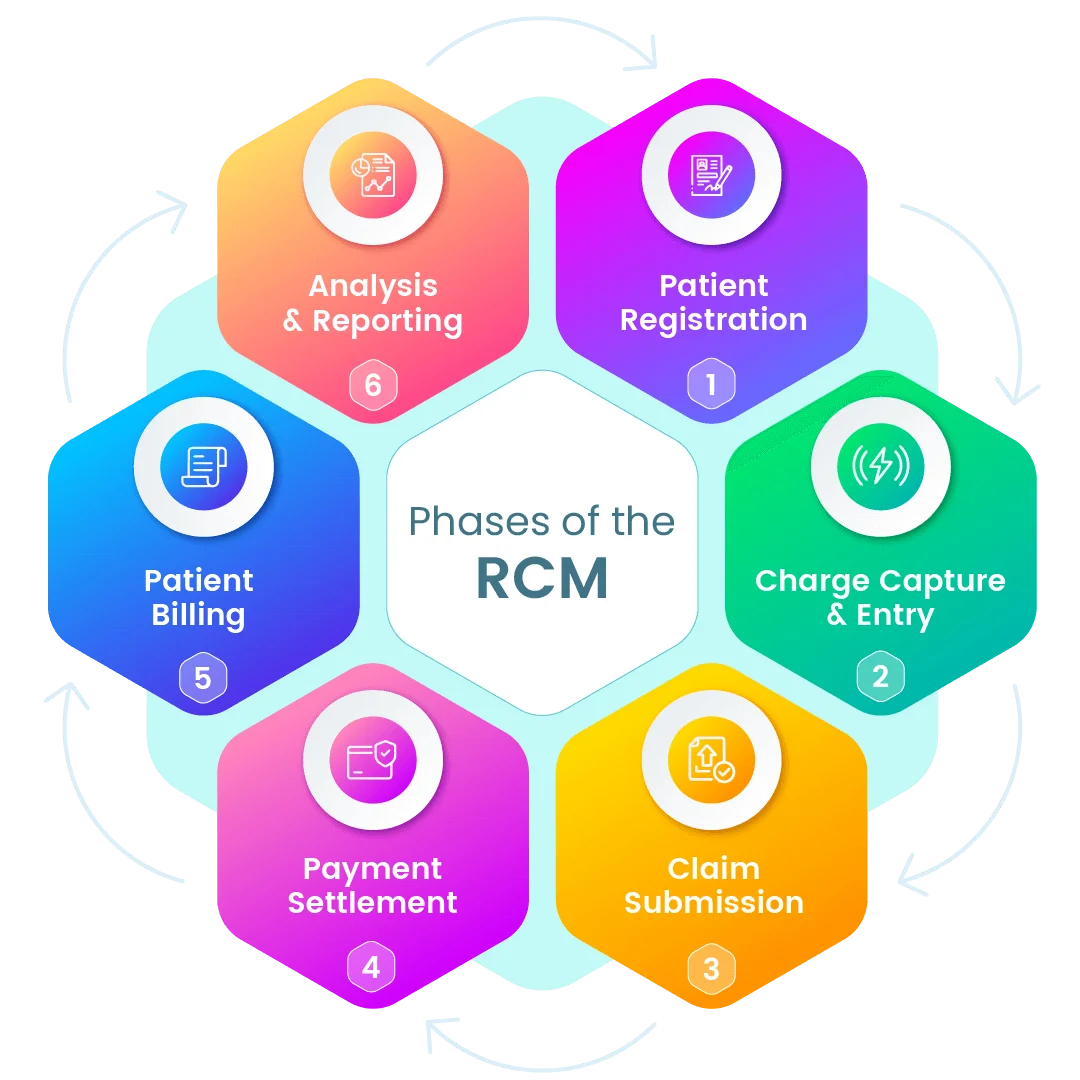
Revenue Cycle Management (RCM) is not a static process. It requires regular attention, assessment, and adjustment to function effectively. This quarterly framework provides a structured, disciplined approach to maintaining financial health through consistent monitoring and strategic improvement.
Quarterly RCM Framework: The 4-Phase Cycle
Q1: Foundation & Benchmarking (January – March)
Begin the year by establishing clarity and solid baselines.
Administrative & Front-End Check
Verify all provider credentials are current and properly loaded in payer portals. Confirm that insurance verification standard operating procedures are being followed for every patient. Review patient registration accuracy metrics, targeting an error rate below 2%. Update all fee schedules in the billing software and conduct staff training on any recent coding or billing updates.
Technology & System Audit
Test all clearinghouse connections and electronic remittance advice (ERA) or electronic funds transfer (EFT) setups. Review the integration points between the EHR, billing, and practice management systems. Confirm backup systems and disaster recovery protocols are functional and audit user access permissions to ensure role-based security.
Performance Benchmarking
Calculate and document first-quarter baseline metrics. Key benchmarks include clean claim rate (target above 95%), days in accounts receivable (target below 40 days), denial rate (target below 5%), and net collection rate (target above 96%). Compare these to industry or specialty benchmarks and identify three to five key areas for improvement in the second quarter.
Q1 Deliverables:
- Current-state RCM assessment report.
- Updated credentialing tracker.
- Staff competency assessment.
- Technology stack evaluation.
- Annual RCM goals document.
Q2: Optimization & Process Improvement (April – June)
Streamline workflows and address the pain points identified in the first quarter.
Denial Management Deep Dive
Analyze the top five reasons for claim denials from Q1. Create or update denial prevention workflows and implement payer-specific rules within the billing software. Establish weekly denial trending reports for ongoing review.
Coding & Documentation Review
Conduct a random chart audit of at least 10-15 charts per provider. Identify any documentation gaps that affect coding accuracy and provide targeted education to providers based on the findings. Review evaluation and management (E/M) coding for compliance with current guidelines.
Patient Financial Experience Assessment
Evaluate the patient billing experience through mystery shopping of calls, portals, and statements. Review the effectiveness of patient payment plans and assess upfront collection processes at registration. Update all financial policy and communication templates as needed.
Mid-Year Financial Health Check
Compare year-to-date performance against annual goals. Review the aging of accounts receivable, with a focus on balances over 90 days. Assess cash flow projections versus actuals and adjust staffing or resources based on volume trends.
Q2 Deliverables:
- Denial root cause analysis report.
- Coding accuracy improvement plan.
- Patient satisfaction survey results.
- Mid-year financial performance review.
- Documentation of implemented process improvements.
Q3: Compliance & Risk Management (July – September)
Ensure regulatory adherence and proactively mitigate financial risks.
Regulatory Compliance Audit
Review updates to the Office of Inspector General (OIG) work plan. Conduct a HIPAA compliance check, with particular attention to remote work environments. Verify Medicare and Medicaid billing compliance and update the organization’s compliance program based on recent enforcement actions.
Payer Contract Review
Analyze the reimbursement terms of the top five payer contracts. Identify any underpayments through contract terms analysis and prepare for upcoming payer negotiations. Verify that all contracted rates are correctly loaded into the billing system.
Internal Controls Assessment
Review the segregation of duties within the revenue cycle. Audit cash handling procedures and review authorization protocols for write-offs and refunds. Assess vendor management practices, especially for any outsourced RCM functions.
Staff Certification & Training
Verify that all billing and coding staff certifications are current. Conduct mandatory compliance training for the team. Assess cross-training needs for key roles and review succession planning for critical positions.
Q3 Deliverables:
- Compliance audit report.
- Payer contract analysis summary.
- Internal controls assessment.
- Staff development and training plan.
- Risk mitigation strategy document.
Q4: Strategic Planning & Forecasting (October – December)
Prepare for the coming year using data-driven insights from the current year.
Annual Performance Analysis
Compare the full year’s performance against the annual goals. Calculate the return on investment for improvement initiatives launched during the year. Analyze seasonal trends and patterns and formally document lessons learned.
Technology Roadmap Planning
Assess any limitations of the current technology stack. Research emerging RCM technologies and create a one- to three-year technology investment plan. Budget for necessary system upgrades or maintenance.
Budget & Forecasting
Develop the RCM department budget for the next fiscal year. Forecast patient volumes based on anticipated provider changes, such as new hires or retirements. Project staffing needs and set Specific, Measurable, Achievable, Relevant, and Time-bound (SMART) goals for the next year.
Vendor & Partner Review
Evaluate the performance of current vendors, including clearinghouses, software providers, and outsourcing partners. Review all service level agreements and conduct a market analysis for potential alternatives. Use performance data as leverage when negotiating contract renewals.
Year-End Close-Out
Perform aggressive follow-up on aged accounts receivable. Review and reconcile all credit balances. Confirm all year-end financial reporting requirements and celebrate the team’s achievements.
Q4 Deliverables:
- Annual RCM performance report.
- Strategic plan for the next year.
- Technology roadmap.
- Approved department budget.
- Vendor partnership assessment.
Monthly Pulse Checks
To maintain momentum between quarterly reviews, implement these regular check-ins.
During the first week of each month, review the previous month’s key performance indicator dashboard. Conduct a leadership team sync on financial performance, review denial trending for the top five reasons, and check the aging of accounts receivable, focusing on balances over 90 days.
In the second week, hold a staff meeting to discuss process challenges and successes. Review payer performance, including reimbursement rates and denial patterns, and conduct a spot check of patient satisfaction.
The third week should focus on cash flow analysis, reviewing any technology issues or updates, and performing a quick compliance check for new regulations.
In the fourth week, prepare for the upcoming quarterly review, celebrate monthly wins, and make any necessary adjustments based on the month’s performance.
Key Performance Indicators to Track
Monitor these critical metrics to gauge financial health:
- Clean Claim Rate: Target above 95%. Track daily or weekly.
- Days in Accounts Receivable: Target below 40 days. Track weekly.
- Net Collection Rate: Target above 96%. Track monthly.
- First-Pass Resolution Rate: Target above 85%. Track weekly.
- Denial Rate: Target below 5%. Track weekly.
- Point-of-Service Collections: Target collecting over 80% of copays and coinsurance at time of service. Track daily.
- Cost to Collect: Target between 4% and 8% of total collections. Track quarterly.
- Patient Satisfaction Score: Target above 90%. Track quarterly.
Implementation Tips
Successfully implementing this framework requires clear ownership. Designate an RCM champion responsible for each quarterly focus area. Leverage technology, such as dashboard reporting, for real-time visibility into performance. Form cross-functional teams that include clinical, administrative, and financial staff in review meetings. Maintain a living RCM playbook that is updated each quarter with lessons learned and process changes. Finally, recognize and celebrate progress to maintain team momentum and engagement.
Conclusion
Adopting a strategic, quarterly approach transforms revenue cycle management from a reactive task into proactive financial stewardship. By systematically addressing different aspects of the revenue cycle throughout the year, healthcare organizations can ensure consistent cash flow, reduce compliance risks, and build a financially sustainable practice.
This framework should be customized to fit an organization’s specific size, specialty, and challenges, but the quarterly rhythm provides a disciplined structure for achieving ongoing RCM excellence.